NHIS saving lives of children with cancer
 NHIS
NHIS
The National Health Insurance Authority (NHIA) in June 2022, added the treatment of the four common childhood cancers to the National Health Insurance Scheme (NHIS) Benefit Package.
These are Acute Lymphoblastic Leukaemia, Burkitt Lymphoma, Retinoblastoma, and Wilms Tumour.
Since its implementation, the childhood cancers policy has been beneficial to many child-patients, despite some few challenges.
The National Health Insurance Authority (NHIA) had conducted initial actuarial modelling of the Scheme’s capacity to absorb the costs of coverage for these childhood cancers with the hope of removing this financial barrier.
It was in this light that the First Lady Rebecca Akuffo-Addo, announced the inclusion of the four most common childhood cancers at the official launch of the nationwide NHIS Week celebrations in November 2021.
This is evidenced by the submission of claims by credentialled healthcare service providers for services rendered to child-patients of cancer, who are active members of the NHIS.
It is the view of the NHIA that the coverage of the four common childhood cancer services was in response to a real need for access to services for a condition that if treated well, could save precious lives who would contribute to the nation’s fortunes.
The NHIA indicates that its commitment toward this goal attainment is unwavering, adding that all measures will be employed to ensure its full implementation in collaboration with the appropriate stakeholders.
Genesis
The NHIA initiated processes, as per its benefit package review guidelines, for the assessment and operationalisation of new benefits and these processes involved the mapping out of reimbursable management pathways, development of reimbursement protocols, costing of services as well as tariff development and final actuarial and budget impact analysis.
The mapping out of the management pathway for childhood cancers and the development of reimbursement protocols was carried out by a multi-stakeholder group of paediatric oncologists involved in the direct care of cancer patients from Korle Bu, Cape Coast, Komfo Anokye, Ho and Tamale Teaching Hospitals; as well as the Geater Accra Regional Hospital and Holy Family Hospital, Techiman.
The others were officials from the Ministry of Health, Ghana Health Service, Health Facilities Regulatory Authority and the National Health Insurance Authority.
The NHIA was also informed that these services were provided by a multi-disciplinary team of experts in only seven facilities: Korle Bu, Cape Coast, Komfo Anokye, Ho and Tamale Teaching Hospitals, plus the Greater Accra Regional Hospital and Holy Family Hospital, Techiman.
This informed the roll-out of coverage in these facilities until the appropriate specialists and equipment were made available in other facilities nationwide.
Since its implementation in June 2022.
The following Claims have been submitted to NHIA for reimbursement:
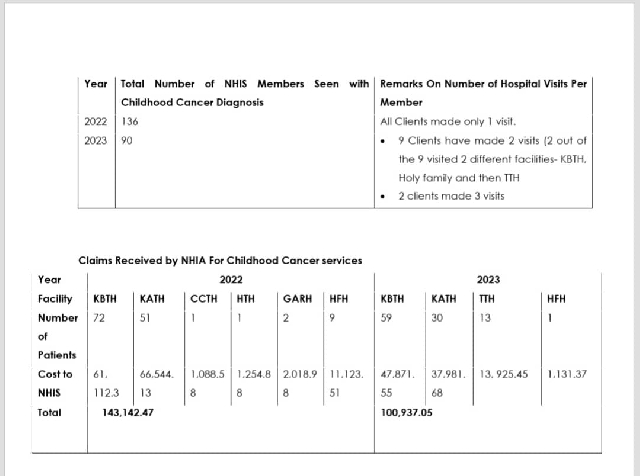
Despite the amounts paid above toward the reimbursement of childhood cancer services, the NHIA is aware of changing economic conditions that warrant reviews of its prices and tariffs.
Service tariffs and medicine prices were, thus, reviewed in February 2023 before the annual due date of July in response to changes in prices.
These price reviews apply to all other services on th benefit package and is an annual periodic activity that is done in collaboration with stakeholders.
The NHIA is currently in the process of comprehensively reviewing its tariff building blocks to arrive at tariffs that will further support the viability of facilities while also ensuring the continued sustainability of the scheme.
The NHIA takes note of claims from facilities of non-availability of medicines and consumables at stated prices and will endeavor to engage relevant stakeholders and regulators of the supply chain to purchase healthcare in the most cost-effective manner to ensure quality healthcare services are made accessible to all members of the scheme.
The NHIA values the distinctive role the mass media, members of the scheme, patient support groups and clinicians play in representing the interest of the populace on health issues and further suggests holistic representation of the efforts being made by the scheme towards providing financial risk protection against the cost of quality healthcare services.








